Imagine drinking a glass of fresh grapefruit juice for breakfast, feeling energized and healthy. Later that day, you take your prescribed blood pressure medication. Hours later, you feel dizzy, flushed, or worse-your heart starts racing uncontrollably. This isn't a hypothetical horror story; it is a real, documented medical emergency caused by one of the most significant drug-food interactions in modern medicine.
The culprit? Grapefruit contains compounds that disrupt how your body processes certain medications. Specifically, when combined with calcium channel blockers, a common class of drugs used to treat high blood pressure, grapefruit can turn a safe dose into a toxic overdose. This interaction was first identified in 1989, yet millions of patients remain unaware of the risk. If you take these medications, understanding this mechanism could save your life.
How Grapefruit Disrupts Your Medication
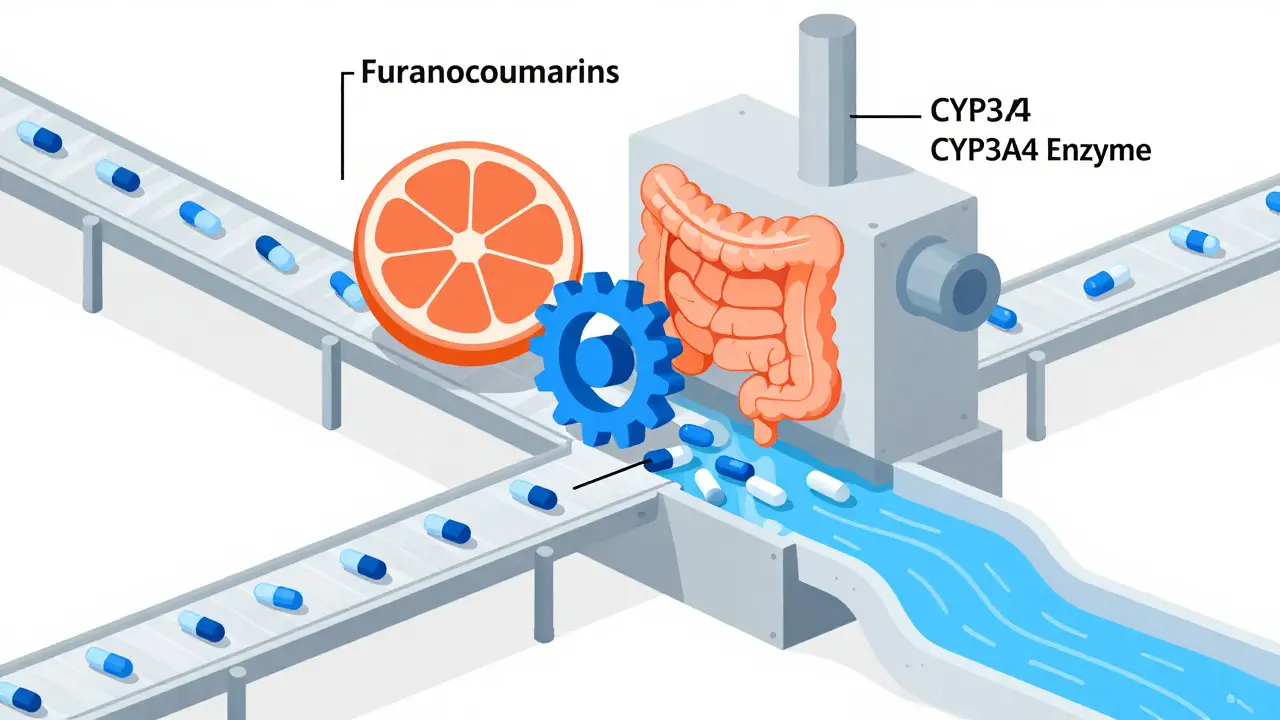
To understand why this happens, we need to look at what occurs inside your intestines. When you swallow a pill, it doesn't go straight into your bloodstream. It passes through your digestive system, where enzymes break down the drug before it reaches your circulation. One specific enzyme, known as CYP3A4 (cytochrome P450 3A4), plays a major role in metabolizing many medications, including calcium channel blockers.
Grapefruit contains natural chemicals called furanocoumarins, specifically bergamottin and 6',7'-dihydroxybergamottin. These compounds act like a key that jams the lock of the CYP3A4 enzyme. Unlike temporary inhibition, furanocoumarins cause irreversible damage to the enzyme in the intestinal lining. Your body has to grow new cells to replace the damaged ones, a process that takes up to 72 hours.
When the enzyme is blocked, the drug bypasses its normal breakdown process. Instead of being partially metabolized and excreted, a much larger amount of the active drug enters your bloodstream. Research shows that a single 200ml glass of grapefruit juice can increase the bioavailability of certain calcium channel blockers by 300% to 500%. For context, if you are supposed to receive 10mg of a drug, you might effectively end up with 40mg or more circulating in your system.
Which Calcium Channel Blockers Are Most Dangerous?
Not all blood pressure medications react to grapefruit in the same way. Calcium channel blockers fall into two main categories: dihydropyridines and non-dihydropyridines. The risk varies significantly between them based on how heavily they rely on the CYP3A4 enzyme for metabolism.
| Medication Name | Type | Risk Level | Primary Effect |
|---|---|---|---|
| Felodipine | Dihydropyridine | High | Up to 500% increase in bioavailability |
| Nimodipine | Dihydropyridine | High | Significantly altered pharmacodynamics |
| Nicardipine | Dihydropyridine | High | Increased plasma concentrations |
| Amlodipine | Dihydropyridine | Moderate | Some interaction, but less pronounced |
| Verapamil | Non-Dihydropyridine | Low/Moderate | Less clinically significant interaction |
| Diltiazem | Non-Dihydropyridine | Low/Moderate | Minimal risk compared to DHPs |
Felodipine is perhaps the most sensitive. Studies have shown that peak plasma concentrations can jump from 2.5 ng/mL to 11.5 ng/mL when taken with grapefruit juice. Even Amlodipine, which is often considered safer, still carries some risk. While the magnitude is lower than with Felodipine, individual variations in metabolism mean that "low risk" does not mean "no risk." Non-dihydropyridines like Verapamil and Diltiazem are generally safer, but caution is still advised.
The Myth of Timing: Why Separating Doses Doesn't Work
A common misconception among patients is that timing can mitigate the risk. Many believe that if they take their medication in the morning and eat grapefruit in the evening, they will be safe. This logic fails because of the duration of the enzyme inhibition.
The furanocoumarins in grapefruit do not just block the enzyme for an hour or two. They cause irreversible inactivation. As noted by Dr. Amelie Hollier, after consuming grapefruit, a significant portion of the drug remains unmetabolized. By day four, an intended 60 mg dose could effectively behave like a 140 mg dose due to accumulated unprocessed drug in the system. The effect lasts up to 72 hours. This means that eating grapefruit three days ago can still impact today's medication dose.
David Bailey, MD, professor emeritus of clinical pharmacology, emphasizes that the greatest hazards come from repeated consumption. Eating grapefruit daily keeps the intestinal enzymes suppressed continuously, leading to a steady rise in drug levels in the blood. There is no "safe window" for taking these specific medications if you consume grapefruit regularly.
Symptoms of Toxicity: What to Watch For
When too much calcium channel blocker enters your system, your blood vessels dilate excessively. This leads to a dangerous drop in blood pressure, known as hypotension. Your body tries to compensate, which can cause a cascade of unpleasant and potentially life-threatening symptoms.
- Severe Dizziness: Feeling lightheaded or faint, especially when standing up quickly.
- Peripheral Edema: Swelling in the ankles, feet, or legs due to fluid retention.
- Flushing: Unexplained redness and warmth in the face or neck.
- Tachycardia: A rapid or pounding heartbeat as the heart struggles to maintain blood flow against low pressure.
- Syncope: Fainting spells, which are particularly dangerous for elderly patients who may fall and sustain injuries.
In severe cases, this interaction can lead to shock or cardiac arrest. Elderly patients are at higher risk because their bodies already process drugs more slowly, and they may have reduced kidney function, compounding the toxicity.
Is All Citrus Fruit Dangerous?
Not all citrus fruits contain furanocoumarins. The risk is highly specific to certain types. Regular sweet oranges, lemons, and limes do not contain significant amounts of these inhibitors and are generally safe to consume with calcium channel blockers.
However, you must be careful with other varieties. Seville oranges, often used in marmalades, contain furanocoumarins similar to grapefruit. Tangelos, a hybrid of tangerine and grapefruit, also pose a risk. Pomelos are another fruit that shares this dangerous chemical profile. Always check the label if you are buying juice blends, as "citrus blend" juices often include grapefruit or Seville orange components.

Safer Alternatives for Hypertension Management
If you love grapefruit and cannot give it up, talk to your doctor about switching medications. There are several classes of antihypertensive drugs that do not interact with grapefruit because they are not metabolized by the CYP3A4 enzyme.
- ACE Inhibitors: Drugs like Lisinopril (Zestril) are commonly prescribed and do not interact with grapefruit.
- Angiotensin-Receptor Blockers (ARBs): Medications such as Valsartan (Cozaar) offer a safe alternative.
- Thiazide Diuretics: Hydrochlorothiazide (Microzide) works by removing excess fluid and is unaffected by citrus.
- Beta-Blockers: Some beta-blockers, like Metoprolol (Lopressor), are safe, though others may have different interaction profiles.
Never switch medications on your own. Your doctor needs to evaluate your overall health, kidney function, and other conditions to choose the right alternative. Recent research is also looking into novel extended-release formulations of amlodipine that show 70% reduced interaction potential, offering hope for patients who need both the drug and the fruit.
Why Doctors Often Miss This Warning
Despite the clear evidence, this interaction is widely underappreciated. A 2022 survey found that only 37% of primary care physicians routinely screen for grapefruit consumption when prescribing calcium channel blockers. Furthermore, 68% of patients were unaware of the risk. This gap in communication is dangerous. Patients often view grapefruit as a superfood, rich in vitamin C and antioxidants, without realizing it acts as a potent pharmaceutical inhibitor.
The prevalence is staggering. Approximately 40% of the 80 million Americans taking calcium channel blockers are affected by this potential interaction. The CDC reports an estimated 15,000 emergency department visits annually related to food-drug interactions involving grapefruit. These numbers highlight a critical failure in patient education.
Can I eat grapefruit if I take Amlodipine?
While Amlodipine has a lower risk profile compared to Felodipine or Nimodipine, it still interacts with grapefruit to some degree. The interaction is less pronounced, but individual metabolism varies. It is safest to avoid grapefruit entirely or consult your doctor for a medication that has zero interaction risk, such as an ACE inhibitor.
How long does the grapefruit effect last?
The inhibitory effect of grapefruit on the CYP3A4 enzyme can last up to 72 hours. Because the enzyme damage is irreversible until new cells are produced, separating the time you eat grapefruit and take your medication does not prevent the interaction. Repeated daily consumption maintains the suppression.
Are organic grapefruits safer?
No. The furanocoumarins responsible for the interaction are naturally occurring compounds within the fruit itself, not pesticides or additives. Organic grapefruit contains the same levels of these inhibitors as conventional grapefruit and poses the same risk.
What should I do if I accidentally ate grapefruit and took my medication?
Monitor yourself closely for symptoms such as dizziness, flushing, swelling in the ankles, or a rapid heartbeat. If you experience severe symptoms like fainting or chest pain, seek emergency medical attention immediately. Inform the medical staff about the grapefruit consumption so they can adjust treatment accordingly.
Does grapefruit juice affect all blood pressure medications?
No. The interaction is specific to drugs metabolized by the CYP3A4 enzyme, primarily certain calcium channel blockers. Other classes like ACE inhibitors (e.g., Lisinopril), ARBs (e.g., Valsartan), and thiazide diuretics are generally not affected by grapefruit.







Anthony Red May 16, 2026
Hey everyone, just wanted to share that my dad actually had a scare with this last year. He was on Felodipine and thought it was fine to have grapefruit juice every morning because he heard it was good for cholesterol. 😅 Turns out the enzymes in his gut were basically jammed shut for days after each glass. His doctor switched him to Lisinopril and now he’s totally safe to eat whatever citrus he wants. It’s wild how much we still don’t know about these interactions until something goes wrong. Hope this helps anyone who’s unsure! 🍊💊
Javier Arauz May 16, 2026
This is exactly why I hate when big pharma pushes these complex drugs instead of just telling people to fix their diet and lifestyle. You’re out there spending hundreds a month on pills that turn into poison if you look at them wrong, all because the system is broken. They want you dependent and scared. Wake up people. Stop trusting these corporate health narratives and take control of your own body naturally before they kill you with a simple fruit. 🇺🇸👎
Kris Wong May 17, 2026
Did you guys realize that the FDA knew about this since 1989 and did absolutely nothing? 🤔 The fact that they let millions of people walk around with potential heart attacks waiting to happen is not an accident. It’s part of a larger plan to keep us sick and dependent on their medical industrial complex. The furanocoumarins are just a cover story for something else entirely. Stay woke. 👁️🍊💀
Danny S May 19, 2026
The so-called 'medical community' is deliberately withholding the truth about natural remedies while pushing synthetic poisons. :-( Grapefruit has been used for centuries without issue until they decided to patent blood pressure meds. This is classic chemtrail-style population control via food interaction suppression. Do your own research and don't trust the mainstream narrative. They want you weak and compliant. :-)
Jeremiah Cassandra May 20, 2026
Oh, brilliant article. Truly groundbreaking discovery that fruit affects digestion. 🙄 I’m sure the doctors are thrilled they didn’t think to mention this when prescribing life-saving medication. But hey, at least we can blame the grapefruit for everything now. Maybe next time we’ll find out that breathing air interacts with our inhalers. Thanks for the shocker, really needed that in my day. 🍊📉
charles robert May 21, 2026
In the grand tapestry of existence, we are merely vessels for chemical reactions we do not understand. 🌀 The grapefruit does not attack; it simply reveals the fragility of our constructed realities. To rely on external substances for internal balance is the ultimate illusion. We fear the fruit because it mirrors our own chaotic nature. The enzyme is not broken; it is awakening. 🍊🌌💭
Warren Brewer May 22, 2026
I read this and thought wow that is scary. My mom takes Amlodipine and she loves grapefruit. I told her to stop eating it right away. She said she would ask her doctor first but I think she should just switch to apples. Apples are safe and healthy too. Good info thanks for sharing.
Mark Ronson May 24, 2026
It is crucial to note that while the interaction is real, individual metabolism varies greatly. As a pharmacist, I often see patients who are unaware of this specific contraindication. Please consult your healthcare provider before making any changes to your medication regimen. There are many alternatives available such as ACE inhibitors which do not have this interaction. Safety first always. 🩺✅
Mikey Mann May 25, 2026
Look, life is full of surprises, even in our breakfast fruits. But instead of fearing the unknown, let's embrace the knowledge. Knowing this doesn't mean you have to give up joy, just adjust your approach. Talk to your doc, maybe try a different med, or just swap the juice for orange. Small changes can lead to big peace of mind. You've got this! 🍊✨💪
Mollie Louise May 25, 2026
I was so excited to see this post because I have been feeling dizzy lately and I drink grapefruit juice every single morning! 🍊😱 I am on Nimodipine for my blood pressure and I never once thought about this connection. I am going to call my doctor immediately to get my levels checked and possibly switch medications. Thank you so much for sharing this important information, it could literally save lives! Let's spread the word to our friends and family too! 💖🏥📢