Have you ever run your hand over your face or the back of your hand and felt a patch of skin that feels like sandpaper? That rough, gritty texture might not just be dry skin. It could be an early warning sign from your body. This condition is called Actinic Keratosis is a precancerous skin condition characterized by rough, scaly patches that develop on sun-exposed skin due to cumulative ultraviolet (UV) radiation damage. Also known as Solar Keratosis, it represents the most common form of skin precancer, affecting millions of people annually. If you notice these rough spots, understanding what they are and how to treat them is crucial for preventing more serious health issues down the road.
What Exactly Is Actinic Keratosis?
Think of your skin as a record of your sun exposure history. When you spend years in the sun without proper protection, the DNA in your skin cells gets damaged. Over time, this damage can cause cells to grow abnormally. These abnormal growths are what we call actinic keratoses. They usually appear on areas that see the most sunlight, like the face, ears, scalp, neck, forearms, and backs of the hands. The American Academy of Dermatology Association notes that approximately 58 million Americans are affected by this condition every year.
Visually, these lesions can be tricky to spot at first. They often start as tiny, rough spots that are more easily felt than seen. As they develop, they can become red, pink, skin-colored, gray, yellow, brown, tan, or even silvery. For patients with darker skin tones, these lesions might look more like age spots or dark patches. The size can vary significantly, ranging from tiny dots to patches up to an inch in diameter. What makes them distinct is the texture. They feel crusty or scaly, and sometimes they can develop into horn-like projections, which signals a higher risk of progression.
The Precancer Connection: Why It Matters
The term "precancerous" is the most critical part of this diagnosis. It means these spots have the potential to turn into invasive skin cancer if left untreated. Specifically, actinic keratoses are linked to cutaneous squamous cell carcinoma. According to DermNet NZ, about 10-15% of patients with more than 10 actinic keratoses will develop squamous cell carcinoma at some point. Without treatment, individual lesions have a 5-10% chance of progressing to cancer over a decade. For immunosuppressed patients, this risk jumps significantly to around 25%.
Medical experts emphasize that treating these lesions is essentially treating early skin cancer. Dr. Henry W. Lim, Chairman of Dermatology at Henry Ford Health System, notes that 90% of cutaneous squamous cell carcinomas originate from untreated actinic keratoses. This statistic highlights why ignoring a rough patch is dangerous. The goal is to stop the progression before the cells invade deeper layers of the skin. Early detection and intervention prevent invasive cancer in nearly all cases, making regular skin checks a vital part of health maintenance.
How Doctors Diagnose the Condition
Diagnosing actinic keratosis is usually straightforward for a board-certified dermatologist. They typically use a technique called Dermoscopy is a non-invasive diagnostic tool that allows dermatologists to examine skin lesions in detail using a magnifying device with light. This method helps them see structures beneath the skin surface that aren't visible to the naked eye. Studies show that dermatologists achieve 95% diagnostic accuracy through visual and tactile examination alone. However, if a lesion looks atypical, feels tender, or has thickness exceeding 0.5 cm, a biopsy might be performed to rule out early squamous cell carcinoma.
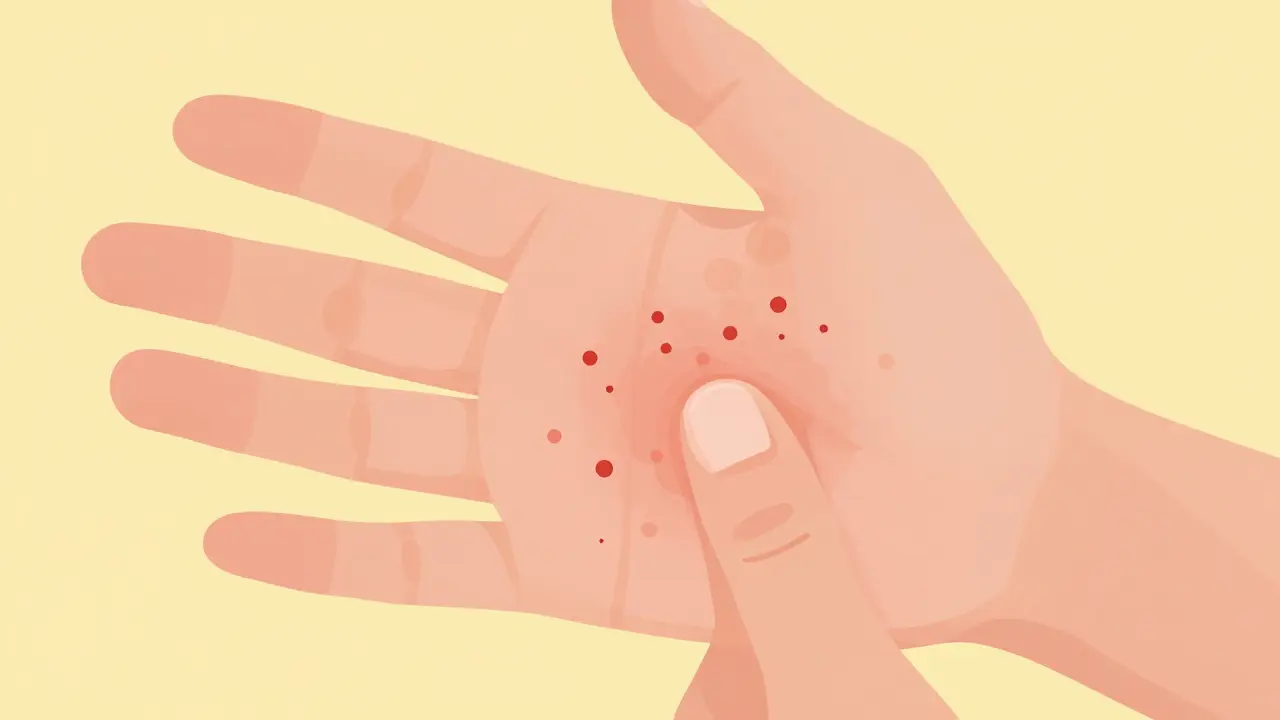
Self-detection plays a huge role, too. About 78% of actinic keratoses are first noticed by patients themselves. The "sandpaper test" is a common method people use: simply running your fingers over sun-exposed areas to feel for rough patches. If you find multiple lesions, don't panic, but do schedule an appointment. Approximately 60% of patients present with multiple lesions, averaging 7-10 spots per person. Early identification allows for simpler, less invasive treatment options.

Understanding Field Treatments
When you have widespread actinic keratoses, treating each spot individually with freezing or scraping can be time-consuming and painful. This is where the concept of field treatment comes in. The skin around a visible lesion often has invisible damage from the sun, a phenomenon known as "field cancerization." Field treatments address the entire affected area, not just the visible bumps. This approach treats both the lesions you can see and the subclinical damage in the surrounding skin.
Field therapy is the standard of care for widespread cases. It reduces the risk of new lesions forming in that area and lowers the chance of cancer development. The Skin Cancer Foundation identifies three primary categories for these treatments: topical medications, chemical peels, and energy-based devices. Choosing the right one depends on the number of lesions, their location, and your skin type. For example, treating the face requires different considerations than treating the scalp or hands.
Common Treatment Options and Comparisons
There are several effective medical treatments available for managing actinic keratosis. Each has its own mechanism, duration, and side effect profile. Below is a comparison of the most common field treatments used in dermatology clinics today.
| Treatment Type | Duration | Clearance Rate | Key Benefit |
|---|---|---|---|
| 5% Fluorouracil is a topical chemotherapy medication that kills rapidly dividing skin cells | 2-4 weeks | 75-85% | Highly effective, generic cost |
| Imiquimod is an immune response modifier that stimulates the body's immune system to fight abnormal cells | 16 weeks | 54-75% | Boosts local immunity |
| Tirbanibulin is a newer topical treatment that disrupts microtubule formation in cancer cells | 5 days | 44% | Shortest treatment course |
| Photodynamic Therapy is a procedure using light and a photosensitizing agent to destroy abnormal cells | 1-2 sessions | 44-75% | Good for large areas |
Fluorouracil is a classic choice, often used for 2 to 4 weeks. It works by interfering with the DNA of the abnormal cells, causing them to die. While effective, it can cause significant inflammation. Imiquimod works differently by stimulating your immune system to attack the lesions, but it requires a longer commitment of up to 16 weeks. Tirbanibulin is a newer option approved by the FDA in 2020. Its biggest selling point is the treatment duration; you only apply it for 5 days, making it more convenient for many patients, though it comes at a higher cost.
Photodynamic therapy involves applying a solution that makes the skin sensitive to light, followed by exposure to a specific light source. This activates the solution to destroy the precancerous cells. It is often chosen for larger areas of the face or scalp. Cryotherapy, or freezing, is another option but is typically used for spot treatment rather than field therapy. It involves applying liquid nitrogen to freeze the lesion, causing it to blister and fall off.

What to Expect During Treatment
It is important to manage your expectations before starting field therapy. These treatments are designed to cause inflammation. When you use creams like fluorouracil, the skin will likely become red, swollen, crusty, and sore. This reaction is actually a good sign; it means the medication is working and the abnormal cells are dying. About 61% of patients undergoing fluorouracil treatment require temporary discontinuation due to severe erythema and crusting. Patients often describe a burning sensation, especially when the cream is first applied.
The recovery phase can be uncomfortable. You might experience peeling or oozing. It is crucial to follow your dermatologist's aftercare instructions, which usually involve keeping the area clean and avoiding sun exposure. Many patients report that the discomfort is worth it to stop cancer before it starts. One patient documented complete lesion clearance after 16 weeks of treatment, noting that the temporary redness was a small price to pay for long-term health. However, 42% of users in online reviews mention "intense burning" during the inflammatory phase, so be prepared for this.
Prevention and Long-Term Care
Treating existing lesions is only half the battle. Preventing new ones from forming is equally important. The most effective strategy is rigorous sun protection. This means wearing broad-spectrum sunscreen with an SPF of 30 or higher every day, even when it is cloudy. You should also wear protective clothing, wide-brimmed hats, and seek shade during peak sun hours. Data from the Skin Cancer Foundation shows that patients who receive structured sun protection counseling reduce new AK development by 37% over 2 years.
Regular monitoring is essential. High-risk patients, such as those with fair skin or a history of severe sunburns, should have annual skin exams. Some dermatology practices now use total body photography to create a baseline, making it easier to spot new changes. If you notice a lesion changing rapidly, becoming tender, or ulcerating, seek medical attention immediately. These are warning signs that a lesion might be progressing to squamous cell carcinoma.
Frequently Asked Questions
Can actinic keratosis go away on its own?
While some lesions may appear to fade, they rarely disappear completely without treatment. Because they are precancerous, leaving them untreated carries a risk of progression to skin cancer. Medical intervention is recommended to ensure they are fully resolved.
How long does it take to recover from field treatment?
Recovery time varies by treatment type. Topical creams like fluorouracil may cause inflammation for several weeks after application stops. Tirbanibulin has a shorter course of 5 days, with recovery typically taking 2-3 weeks. Photodynamic therapy recovery is usually about 1 week.
Are field treatments painful?
Field treatments often cause discomfort, including burning, stinging, and redness. This is a normal part of the healing process as the medication targets abnormal cells. Pain management strategies, such as cool compresses or prescribed creams, can help manage symptoms.
Can I use sunscreen during treatment?
Yes, sun protection is critical during treatment. However, you should consult your doctor about which sunscreen is best, as some ingredients might interact with topical medications. Generally, mineral-based sunscreens are safer for irritated skin.
Why do I need to treat the whole area instead of just the spots?
Treating the whole area addresses "field cancerization," where invisible damage exists in the skin around visible lesions. Field treatments reduce the risk of new lesions forming in that specific area, offering better long-term protection than spot treatment alone.





Marissa Staples March 26, 2026
It is wild how much our skin remembers everything we have done.
I never thought about the sandpaper feeling being a warning sign until now.
It makes me wonder about all the days I spent outside without a hat.
We really treat our bodies like they are disposable sometimes.
The idea of field cancerization is pretty haunting when you think about it.
You can see the damage but not the invisible stuff underneath.
It feels like a metaphor for how we handle other things in life.
Prevention is always better than cure but nobody wants to hear that.
Reading about the treatment options made me realize how much pain people go through.
Inflammation is the body fighting back and that is a strange concept.
I guess I need to start checking my hands more often.
It is easy to ignore small changes until they become big problems.
The statistics about squamous cell carcinoma are definitely not comforting.
I hope people take this seriously before it is too late.
Maybe we should all just wear long sleeves more often.
It is a small change that could save a lot of trouble later.
Stephen Alabi March 27, 2026
The diagnostic process involves more complexity than visual inspection alone.
Dermoscopy is not always sufficient for every case of atypical lesions.
One must consider the limitations of visual examination in diverse skin tones.
The text suggests a high accuracy rate which is debatable in clinical practice.
It is imperative to understand that biopsy remains the gold standard for certainty.
Ignoring the nuances of histopathology leads to misdiagnosis.
The treatment protocols mentioned are standard but not universally applicable.
Patients should not rely solely on topical agents for advanced cases.
The narrative here lacks critical depth regarding systemic implications.
Medical literature requires a more rigorous approach than this summary provides.
I find the casual tone inappropriate for such a serious medical condition.
It is necessary to maintain professional standards in health communication.
Agbogla Bischof March 28, 2026
You make some valid points regarding histopathology!! However, the article aims for general public education! ; The accuracy rates cited are from peer-reviewed studies! We must not discourage people from seeking initial screening! ; Dermoscopy is indeed a first-line tool for efficiency! It is important to balance technical precision with accessibility! ; Many patients cannot afford immediate biopsies for every spot! Early detection saves lives even with visual checks! ; The text does mention biopsy for atypical lesions clearly! We should support the message of prevention rather than critique the medium! ; Your formal tone might alienate the average reader! Knowledge should be shared in an understandable way! ; Thank you for adding your expertise to the discussion! It helps clarify the medical standards involved! ; We all want better health outcomes for everyone! ;
Elaine Parra March 28, 2026
This is exactly why American healthcare is failing so many people.
We ignore the sun until it burns us completely.
Other countries prioritize skin health much better than we do here.
The cost of treatment is ridiculous compared to prevention.
People need to stop being lazy about sunscreen application.
It is unacceptable that so many wait until cancer forms.
We need stricter regulations on outdoor activities during peak hours.
The government should mandate protective clothing for workers.
Ignoring these warnings is a failure of personal responsibility.
This post should have been more aggressive about the risks.
We are playing with fire every time we step outside unprotected.
Stop making excuses about vitamin D and just protect your skin.
This is a national health crisis that we are ignoring.
Katie Putbrese March 29, 2026
It is your duty to protect your body as a gift from above.
Neglecting your health is a moral failing that affects your family.
We must all take responsibility for our own actions regarding the sun.
Shame on those who refuse to wear hats or sunscreen.
It is selfish to risk cancer and burden the healthcare system.
You should feel guilty if you ignore these clear warning signs.
Discipline is required to maintain proper health standards.
We need to stop blaming the system and start fixing ourselves.
This is a test of character for every single person.
Do not wait for a doctor to tell you to change your habits.
The consequences of laziness are too severe to ignore.
We must uphold the highest standards of self-care always.
peter vencken March 30, 2026
i went through this last year and it was a nightmare.
the burning sensation is real and nothing prepares you for it.
i used the cream for like 3 weeks and my face looked awful.
but now everything is clear and i feel so much better.
sunscreen is a must every single day no matter what.
dont skip it even when its cloudy outside.
the dermatologist said i was lucky to catch it early.
hope everyone here stays safe and checks their skin.
its scary but treatable if you act fast.
just listen to the pros and dont ignore the spots.
take care of yall.
Kevin Siewe April 1, 2026
I am glad you are feeling better now.
It takes courage to go through that treatment process.
You are an inspiration to others who might be hesitant.
Please keep up the good work with your aftercare.
Your experience helps validate the importance of early detection.
Stay strong and continue to protect your skin.
We are all rooting for your continued health.
It is wonderful to hear about a successful recovery.
You handled the situation with great resilience.
Keep prioritizing your well-being moving forward.
Linda Foster April 3, 2026
Regular skin examinations remain a critical component of preventative health measures.