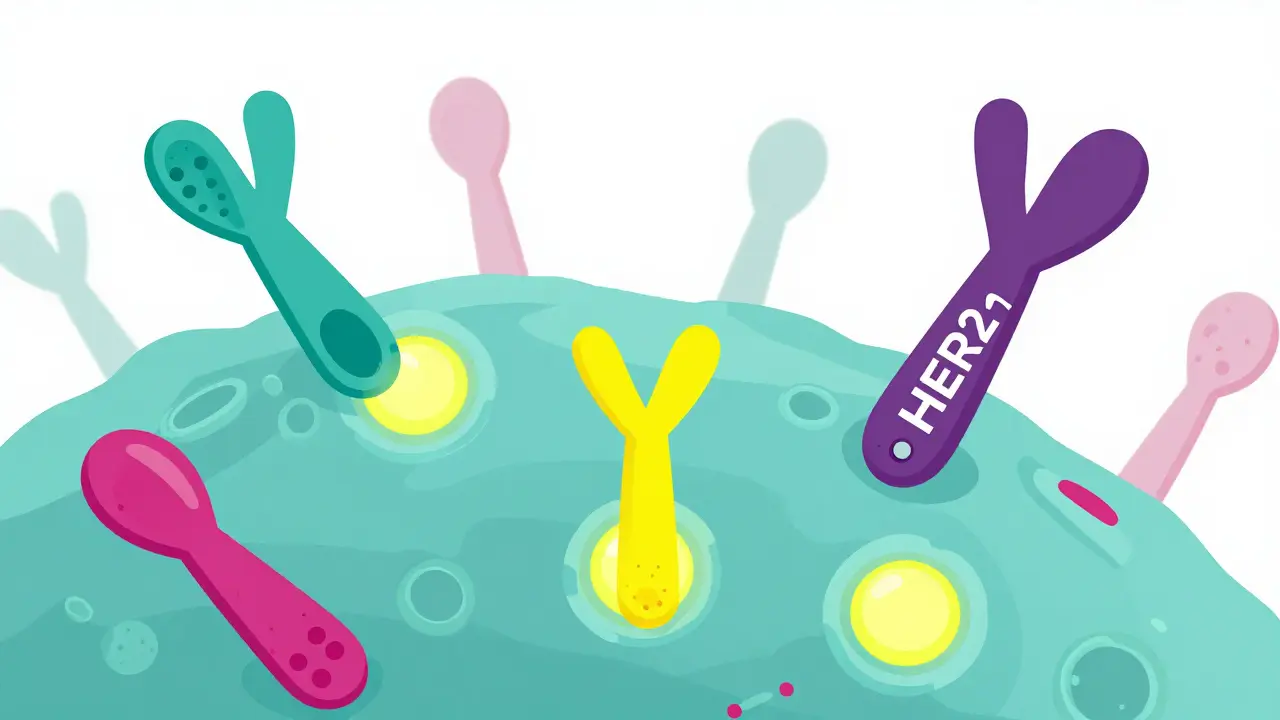
Imagine a protein on the surface of a cell that acts like an "on" switch for growth. In some breast cancers, this switch is stuck in the "on" position because the cell produces too much of a specific protein called HER2-positive breast cancer is a molecular subtype of breast cancer characterized by the overexpression of the human epidermal growth factor receptor 2 (HER2) protein, which drives aggressive tumor growth. This isn't your typical breast cancer; it's faster and more aggressive, affecting about 15% to 20% of patients. But here is the good news: because we know exactly what is driving the growth, we can use precision medicine to shut that switch off.
What exactly are targeted therapies?
Unlike traditional chemotherapy, which attacks all fast-growing cells (including healthy ones like your hair follicles), targeted therapies are like guided missiles. They are designed to find and bind to specific markers on cancer cells. In this case, they target the HER2 protein, blocking the signals that tell the tumor to multiply. This shift in approach has turned one of the most feared diagnoses into a manageable condition with significantly better survival rates.
The Heavy Hitters: Main Types of HER2 Drugs
Not all targeted drugs work the same way. Doctors usually categorize them into three main groups based on how they attack the cancer.
Monoclonal Antibodies
These are proteins made in a lab that mimic the body's own immune system. Trastuzumab (often known by the brand name Herceptin) was the first breakthrough here. It sticks to the HER2 receptor and flags the cell for destruction. Another key player is Pertuzumab, which works differently by preventing the HER2 protein from pairing up with other receptors-a process called dimerization. When used together, they create a "dual blockade" that is often more effective for larger tumors.
Antibody-Drug Conjugates (ADCs)
Think of ADCs as a "Trojan Horse." An antibody finds the HER2 protein, but it's carrying a powerful payload of chemotherapy attached to it. Once the antibody enters the cell, it releases the chemo directly inside the tumor. Trastuzumab deruxtecan (Enhertu) is a game-changer in this category. In the DESTINY-Breast03 trials, it showed a 72% reduction in the risk of disease progression compared to older ADCs like T-DM1.
Tyrosine Kinase Inhibitors (TKIs)
While antibodies work on the outside of the cell, TKIs are small molecules that slip inside the cell to block the growth signals from within. Tucatinib is particularly important because it's one of the few drugs capable of crossing the blood-brain barrier, making it a primary choice for patients with brain metastases.
| Drug Class | How it Works | Key Examples | Primary Delivery | Main Advantage |
|---|---|---|---|---|
| Monoclonal Antibodies | Blocks receptor surface | Trastuzumab, Pertuzumab | IV or Subcutaneous | Standard first-line care |
| ADCs | Delivers chemo payload | Trastuzumab deruxtecan (T-DXd) | IV Infusion | Highly potent cell kill |
| TKIs | Blocks internal signals | Tucatinib, Neratinib | Oral Tablet | Crosses blood-brain barrier |
The Shift Toward "HER2-Low"
For years, you were either HER2-positive or HER2-negative. But we've discovered a middle ground called "HER2-low" (where the protein is present but in small amounts). This is a massive deal because it means drugs like T-DXd can now help a much larger group of people-potentially up to 50-60% of metastatic patients-who previously had no targeted options. This expansion is redefining how we classify breast cancer entirely.
Managing the Side Effects
Targeted therapy is generally easier on the stomach and hair than chemo, but it brings its own set of challenges. The biggest concern with drugs like Trastuzumab is cardiotoxicity. About 2% to 7% of patients may experience symptomatic heart failure. This is why your oncologist will order an echocardiogram every few months to check your left ventricular ejection fraction.
Other therapies have different "trade-offs":
- T-DXd: Carries a risk of interstitial lung disease (inflammation of the lung tissue), which can manifest as a persistent cough.
- TKIs: Often cause significant gastrointestinal issues. For example, Neratinib is notorious for causing severe diarrhea, often requiring a strict regimen of loperamide from the first sign of a loose stool.
- Infusion Fatigue: Traditional IV drips can take hours. The introduction of Phesgo-a subcutaneous injection-has reduced some treatment times from 90 minutes to under 10 minutes, which is a huge win for quality of life.
What Does the Treatment Journey Look Like?
Treatment isn't a one-size-fits-all path; it's a sequence designed to keep the cancer at bay as long as possible. For early-stage cancer, the standard is usually a year of Trastuzumab paired with chemotherapy. If the tumor is larger than 2 cm, doctors often start with a dual blockade of Trastuzumab and Pertuzumab before surgery (neoadjuvant therapy).
For metastatic disease, the strategy shifts. You'll typically start with a combination of Trastuzumab, Pertuzumab, and a taxane chemotherapy. If that stops working, the sequence usually moves to T-DM1, and then to high-potency options like T-DXd or tucatinib-based regimens. The goal is always to move to the most powerful tool only when the previous one has been exhausted.

What's Next on the Horizon?
We are moving toward a future where almost every breast cancer patient might receive some form of targeted therapy. The DESTINY-Breast06 trial is currently looking at "HER2-ultralow" patients, which could expand eligibility to 70% of all breast cancer cases. Researchers are also testing bispecific antibodies-drugs that can grab two different receptors at once-and combining these with immunotherapy to make the body's own T-cells fight the tumor more effectively.
Is HER2-positive breast cancer more dangerous than other types?
Historically, yes, because it grows and spreads more quickly. However, because the targeted therapies mentioned above are so effective, the long-term outlook for HER2-positive patients has improved dramatically compared to the era before these drugs existed.
How often do I need heart checks during treatment?
Standard guidelines suggest a baseline heart function test (like an echocardiogram or MUGA scan) before starting Trastuzumab, followed by checks every 3 months during the treatment period to monitor for any decrease in heart pump efficiency.
Can I take these medications at home?
It depends on the drug. Monoclonal antibodies and ADCs usually require a clinic visit for IV infusion or subcutaneous injection. However, TKIs like Tucatinib and Neratinib are oral tablets that you take at home.
What is the difference between HER2-positive and HER2-low?
HER2-positive means the cancer has a high amount of the HER2 protein. HER2-low means there is some protein present, but not enough to be called positive by traditional standards. Recently, drugs like Trastuzumab deruxtecan have proven effective even in HER2-low patients.
Why do some patients get diarrhea from TKIs?
Tyrosine Kinase Inhibitors can affect the lining of the gut and the way fluids are absorbed. This is a common side effect, particularly with Neratinib, and is typically managed with proactive use of anti-diarrheal medications like loperamide.
Next Steps and Support
If you or a loved one has just received a HER2-positive diagnosis, the first step is to confirm the exact HER2 status through IHC (immunohistochemistry) or FISH (fluorescence in situ hybridization) testing. This determines which "bucket" of therapy you fit into. Ask your oncologist about the possibility of subcutaneous options like Phesgo if you are worried about long clinic visits, and ensure a cardiology plan is in place for monitoring. If you experience a new, dry cough while on an ADC, contact your care team immediately to rule out lung inflammation.






dwight koyner April 5, 2026
The distinction between HER2-positive and HER2-low is a critical point for current clinical practice. It is important to note that the transition to using Antibody-Drug Conjugates for the low-expression group represents a paradigm shift in how we approach precision oncology. This allows for a much broader application of targeted agents that were previously restricted to a small subset of patients.
Rupert McKelvie April 7, 2026
It is truly amazing to see how far medical science has come in such a short time. The outlook for patients today is so much brighter than it was even a decade ago.
Daniel Trezub April 9, 2026
Sure, the science sounds great on paper, but let's be real, these "breakthroughs" usually just mean more expensive bills for the patient. The a-ha moment about HER2-low is just a way for pharma to expand their market share to 60% of patients. It is pretty obvious when you look at the pricing models of these new ADCs.
Vivek Hattangadi April 9, 2026
I totally agree that the shift toward HER2-low is a massive deal! It gives so many more people a fighting chance. We should really keep sharing these guides to make sure everyone knows about the different testing options like FISH and IHC so they can advocate for themselves at the clinic!
Michael Flückiger April 9, 2026
Absolutely incredible progress!!! The fact that we can now cross the blood-brain barrier with Tucatinib is just... wow!!! It really gives a lot of hope to people who thought they were out of options!!!
Ethan Davis April 11, 2026
Funny how they just "discover" a new category like HER2-low right when the old patents are expiring. They want us to believe in these guided missiles, but they never talk about the long-term systemic effects of these chemicals on the body. Probably just another way to keep people on a subscription of meds for the rest of their lives.
Stephen Luce April 12, 2026
Reading about the side effects like cardiotoxicity is really sobering. It's a tough trade-off, but having that monitoring in place makes it feel a bit more manageable for those going through it.
Jamar Taylor April 14, 2026
Keep fighting the good fight everyone! Every single one of these new drug classes is a tool in the belt to get back to a normal life. You've got this!
Christopher Cooper April 14, 2026
The mention of Phesgo is actually very significant for the patient experience. Many of us don't realize how much the logistics of treatment-the hours spent in a chair-contributes to the overall mental fatigue of cancer care. Reducing a 90-minute infusion to a 10-minute injection is not just a convenience; it is a substantial improvement in the quality of life.
Furthermore, the development of bispecific antibodies is an intriguing frontier. If we can simultaneously target two receptors, the potential for reducing tumor escape mechanisms is huge. I find it fascinating how we are moving toward a multi-pronged attack. The synergy between immunotherapy and targeted therapy could be the key to turning these manageable conditions into actual cures. It is a complex journey, but the precision is what makes it hopeful. We are essentially moving from a shotgun approach to a sniper approach. This level of specificity reduces collateral damage to healthy tissues. The focus on the blood-brain barrier is also a huge win. For too long, the brain was a sanctuary for cancer cells. Now, we have ways to penetrate those defenses. It is a great time for medical innovation. I hope more people look into the clinical trials mentioned, like DESTINY-Breast06. Access to these trials can be life-changing. It is all about the right drug for the right patient at the right time. The evolution from HER2-positive to HER2-low shows that our understanding of the disease is constantly evolving. We are not just treating a type of cancer; we are treating a specific molecular error. That is the beauty of modern medicine. Keep pushing for the most current data when talking to your doctors. Knowledge really is power in these situations.
Sarabjeet Singh April 15, 2026
Stay strong and keep moving forward.
charles mcbride April 15, 2026
This is such an optimistic look at the current landscape. It's truly heartening to see the options expanding for so many.
Alexander Idle April 17, 2026
Oh, please! This is absolutely catastrophic! The sheer audacity of suggesting that a "persistent cough" is just a side effect when it could be full-blown interstitial lung disease is simply scandalous! I am utterly appalled by the clinical coldness of this layout! It is a tragedy of the highest order!