We've all heard the story: a doctor switches a patient from a brand-name drug to a cheaper generic alternative, and suddenly the symptoms return or new side effects appear. On paper, these medications contain the same active ingredients and meet strict regulatory standards. Yet, the experience of taking them isn't always identical for the patient. This discrepancy points to a powerful psychological phenomenon known as the nocebo effecta phenomenon where negative expectations about a treatment lead to reduced efficacy, worsening of symptoms, or new adverse effects that occur independently from the active treatment component. In 2026, understanding how to manage this dynamic is crucial for healthcare providers and patients alike, especially when navigating the complex relationship between cost-saving measures and patient trust.
The core challenge lies in the gap between chemical equivalence and psychological perception. Even when blood tests confirm that the drug levels are identical, the mind's belief system can alter the physiological response. A significant study published in 2025 demonstrated that participants given a sham treatment associated with generic cues reported significantly more negative outcomes than those given branded cues, despite receiving the same inert substance. This suggests that the "label" we attach to a medicine matters just as much as the chemistry inside the bottle.
Understanding the Nocebo Mechanism
To manage the impact, we first need to understand what happens internally. The term comes from Latin, meaning "I will harm." Unlike the placebo effect, which relies on positive expectation to heal, the Nocebo Effectthe opposite of the placebo effect where negative beliefs cause harmful symptoms or reduce treatment effectiveness operates through anticipatory anxiety. When a patient expects a drug to fail or hurt them, their brain releases stress chemicals that can heighten sensitivity to pain or trigger digestive issues.
This isn't imagination; it's physiology. For instance, researchers at Brigham and Women's Hospital found that negative bias against generics leads to measurable clinical outcomes. In clinical trials, approximately one in five people in the placebo group spontaneously report side effects. These aren't tricks; they are genuine physical sensations driven by the expectation of harm. When you tell someone, "This might give you a headache," you prime their brain to scan for headaches, interpreting normal fatigue or mild discomfort as medication failure.
Why Generic Drugs Trigger Negative Expectations
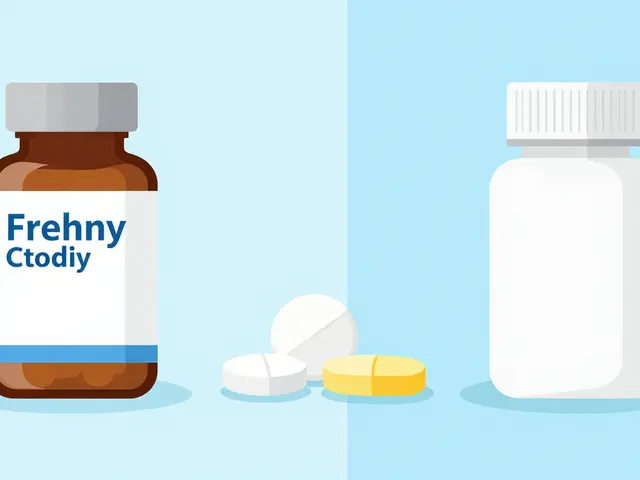
So why does a generic version often spark this reaction while the brand version does not? Several factors converge here. First, there is the issue of trust history. If a patient has had a bad experience with a cheap product in the past, that memory transfers to the new medication. Second, the visual cues play a massive role. In a 2024 experiment involving anti-itch cream, participants told the product was expensive reported fewer side effects than those told it was cheap, even though both tubes contained nothing at all.
- Pricing Signals: Low cost subconsciously signals "lower quality" to many consumers.
- Naming Complexity: Generic labels often feature long, complex chemical names or manufacturer codes compared to the catchy, short names of brands.
- Packaging Differences: Changes in color, size, or texture of pills can signal change, triggering skepticism.
- Media Influence: News stories or social media complaints about switch failures reinforce the fear of generic substitution.
In Australia, where government schemes like the PBS (Pharmaceutical Benefits Scheme) prioritize generics to reduce national healthcare spending, this tension is visible. Patients see the price drop but fear a drop in care. This cognitive dissonance sets the stage for the nocebo effect.
| Factor | Brand-Name Influence | Generic Influence |
|---|---|---|
| Packaging Aesthetics | High quality, consistent branding | Varied, sometimes utilitarian design |
| Name Recognition | Familiar, simple marketing names | Technical, descriptive chemical names |
| Price Anchor | Perceived high value due to cost | Perceived low value due to discount |
| Social Validation | Historically established reputation | Frequently discussed as "inferior" online |
The Role of Packaging and Pricing Signals
We often underestimate how much packaging contributes to efficacy. Neuroscientists have shown that the look of a box can alter the reporting of side effects. In studies where healthy volunteers received a spray labeled as "brand" versus "generic," those given the generic label reported higher rates of nausea and mood changes. They weren't lying; their brains were reacting to the lack of perceived safety.
The mechanism involves heightened awareness. When you expect a generic to be harsh, you monitor your body more closely. You notice a slight stomach rumble and attribute it to the pills rather than dinner. This creates a feedback loop where the medication is viewed as the source of distress. To break this loop, we must address the visual environment. Some pharmaceutical companies are exploring strategies to maintain similar packaging aesthetics for authorized generics-products made by the original brand owner but sold under a generic label-to bridge this perceptual gap without violating antitrust rules.

Communication Strategies for Clinicians
For doctors and pharmacists, the way information is delivered is the most powerful tool. It is not about withholding truth; it is about reframing context. Standard informed consent often lists every possible rare side effect to protect the provider legally. However, listing every worst-case scenario invites the nocebo effect.
A better approach involves focusing on the majority outcome. Instead of saying, "You might get a rash," try, "Most people tolerate this very well, though occasionally some notice minor skin changes." This technique, supported by research from 2023, maintains transparency without planting seeds of anxiety. Building a therapeutic alliance is also vital. When a doctor says, "I chose this medication because it's proven to work just as well," it carries weight. Trust acts as a buffer against negative expectations.
Furthermore, pre-emptive counseling helps. If a patient knows they will be switched to a generic, prepare them beforehand. Explain that the active ingredient is chemically identical. Use the concept of Bioequivalencea requirement that generic drugs demonstrate they deliver the same amount of active ingredient into the bloodstream in the same amount of time as the brand-name drug. Remind them that regulations require the difference in blood concentration to be within a very narrow margin (typically 80-125%), ensuring safety.
Navigating Regulatory Standards and Transparency
Regulatory bodies like the FDA in the United States and the Therapeutic Goods Administration (TGA) in Australia enforce rigorous standards. A generic must prove bioequivalence before approval. Despite this, public perception lags behind science. Part of the solution lies in public health campaigns that explain the approval process. When patients understand the scrutiny involved, the fear factor diminishes.
Data shows that when patients are informed about the cost savings ($3,000+ annually per patient in some estimates) alongside efficacy info, nocebo effects decrease by roughly 37%. Money is a tangible benefit. By linking the financial relief to the safety assurance, clinicians provide a dual-value proposition. The European Medicines Agency (EMA) has also updated guidelines to recommend that packaging differences shouldn't unnecessarily alarm patients, acknowledging that design impacts compliance.

Future Directions and Practical Steps
Looking ahead, we need standardized tools to measure nocebo risk during consultations. Imagine a quick questionnaire that flags patients who are particularly anxious about medication changes so doctors can tailor their explanation. We also need to monitor digital spaces where misconceptions thrive. Reddit and social media groups often amplify isolated bad experiences into generalized fears. Counter-narratives provided by trusted professionals in these forums can help correct the record.
For now, the practical steps remain simple but impactful:
- Educate Early: Explain bioequivalence before dispensing the drug.
- Positive Framing: Focus on the success rate, not just the side effect profile.
- Monitor Closely: Check in after a brand switch to validate any concerns.
- Respect Preferences: If a patient insists on a brand, listen to their reasoning. Sometimes the peace of mind is worth the extra cost.
By acknowledging the power of expectation, we treat the whole person, not just the disease. Chemistry gives us the cure; psychology ensures the patient believes in it.
Frequently Asked Questions
Is the nocebo effect fake?
No. The nocebo effect causes real, measurable physical symptoms. It is not "faking it" but a psychosomatic response where negative expectations trigger stress pathways in the body that manifest as pain, nausea, or other ailments.
Are generic medications actually less effective?
Scientifically, no. Generics must pass strict bioequivalence testing showing they perform the same in the body as brand-name drugs. Any difference in reported effectiveness is often due to patient expectation and perception rather than the chemistry of the drug.
Can packaging really affect how well a drug works?
Yes. Studies suggest that expensive-looking packaging can increase perceived efficacy, while plain packaging may enhance the nocebo effect. Visual cues influence the brain's preparation for the drug, altering the symptom experience.
How can I explain bioequivalence to a skeptical patient?
Explain that regulators check the speed and level of the drug in the blood. The difference allowed is very small (within 20% range). Compare it to buying two different brands of flour or sugar; they cook the same even if the bag looks different.
What should I do if a patient feels worse on the generic?
Validate their concern. Rule out other medical causes. If symptoms persist, it may be best to prescribe the brand-name version if available and covered, or switch to a different manufacturer's generic to rule out inactive ingredient allergies.






Vikash Ranjan March 31, 2026
I am constantly surprised by how easily people accept generic drugs without questioning the manufacturer. You seem to forget that cost cutting often means quality control corners being cut somewhere in the supply chain. It is dangerous to assume chemical equivalence translates perfectly to physiological reality every single time. Your focus on psychology misses the tangible differences in filler materials that trigger reactions. We cannot just wave our hands and say it is all in the head when patients feel real pain. Stop ignoring the industrial flaws that exist beneath the regulatory surface layer.
RONALD FOWLER April 2, 2026
We should focus on understanding rather than fear though. I believe that trust between doctors and patients matters more than the pill color or price tag. Most people feel better when treated with respect instead of being lectured about chemistry facts. Listening helps bridge the gap between what we know and what patients feel. We need patience when discussing these sensitive topics with families.
Carolyn Kask April 3, 2026
Ah yes the standard "trust me bro" approach while the FDA watches quietly. Americans pay too much for brand names and then complain when insurance forces a switch to cheap stuff. Your empathy sounds nice but does not fix the broken pricing model that drives these decisions. We love our regulations yet still wonder why the system fails us so often.
Dan Stoof April 3, 2026
This is such an amazing insight into human psychology!!! Why do we never talk about this enough in medical school?? The power of belief is absolutely incredible and needs to be harnessed better!!! We can change health outcomes just by changing how we speak!!! It feels so good to see science validate what intuition has known for years!!! Let us hope this study helps everyone feel safer about their meds!!!
Ruth Wambui April 4, 2026
Big Pharma knows exactly how to manipulate your brain with packaging colors to keep you buying high margin items. They plant seeds of doubt about generics because cheap competition threatens their billions in profit margins. The visual cues mentioned here are part of a larger design strategy to keep consumers dependent on brands. Do not trust the studies funded by the same companies making the drugs.
Charles Rogers April 5, 2026
You are falling into a classic trap of assuming malice where none exists. Regulatory bodies do perform rigorous testing before approval of new formulations. It is a foolish idea that everything is a plot against the consumer health. Stick to the data presented in peer reviewed journals instead of speculating online.
Brian Yap April 6, 2026
Heres in Australia we deal with the PBS constantly and it works generally well for most blokes. The debate about generic versus brand gets heated down under too but usually settles once you get back to normal life. We appreciate the savings even if the pills look slightly different sometimes.
Katie Riston April 6, 2026
The intersection of material object and subjective experience creates a complex philosophical landscape that we rarely explore deeply enough. When we view the medication as merely a chemical delivery system we miss the ritualistic aspect of healing which involves trust and belief systems entirely. This phenomenon illustrates how the mind constructs reality based on prior expectations rather than objective external stimuli alone. It is fascinating to consider that our biology is not separate from our culture or marketing influences on a fundamental level. The nocebo effect serves as a reminder that healing is a holistic process involving mind body and environment together. We must acknowledge the weight of historical trauma regarding medical care in marginalized communities specifically. Trust is built over generations and lost in moments so the impact of switching medications carries significant social weight. Understanding this requires us to slow down and listen to patient narratives without immediately dismissing them as irrational fears. Science tells us the ingredients are the same but lived experience tells us the outcome can differ due to internal states. We cannot reduce human suffering to mere statistics or bioequivalence margins if we wish to heal effectively. The future of medicine must integrate psychological support alongside pharmacological intervention for best results always. Ignoring the emotional component of treatment leads to poorer adherence rates and worse health metrics overall eventually. We need policies that support the therapeutic relationship as much as the chemical efficacy of treatments available today. This conversation about branding and perception reveals deep truths about how humans value things regardless of utility. The label becomes the medicine in ways that regulators struggle to quantify or measure accurately yet. Ultimately we must treat the person not just the disease process to achieve true wellness outcomes in society.
Beccy Smart April 7, 2026
Glad you posted this because I hate when people pretend generics are magic cures 🙄😤💉💊
Jonathan Alexander April 8, 2026
This is the most important discussion happening right now regarding healthcare access globally. My own experience with a brand switch nearly ruined my confidence in the doctor who prescribed it. The anxiety spirals are real and devastating for those living with chronic conditions daily. We cannot ignore the emotional toll of uncertainty when managing serious illnesses effectively. Every small detail matters when your health hangs in the balance completely.
Christopher Curcio April 9, 2026
Bioavailability metrics such as C-max and AUC are critical factors that determine clinical equivalence beyond simple active ingredient matching. Pharmacokinetic profiling ensures systemic exposure remains consistent across different manufacturing sources. Formulation excipients play a significant role in absorption rates and potential hypersensitivity responses clinically. Therapeutic equivalence indices are established during submission review processes by governing health authorities strictly. Physicians should communicate these parameters clearly to mitigate nocebo activation in vulnerable populations.
Angel Ahumada April 11, 2026
oh please spare me the jargon dump. Real understanding comes from observing behavior patterns not memorizing regulatory acronyms. The common person does not care about AUC values they care about feeling better today. We live in a world where nuance is drowned out by technical language designed to obscure truth. Simple communication yields better compliance than complex lectures ever could have done.
Debbie Fradin April 12, 2026
It is ridiculous how many people claim to be experts on this without ever reading the primary literature themselves. The media narrative pushes generic fear while ignoring the financial necessity for public health systems to function. We need to stop letting anecdotes override population level safety data consistently. Your personal bias is clouding your ability to see the bigger picture of healthcare economics.
Rick Jackson April 14, 2026
We find value in acknowledging both perspectives equally. Data supports safety yet experience validates concern. Balance is key.